How Can You Tell If You Have Shin Splints or a Stress Fracture?
Medial Tibial Stress Syndrome (MTSS) once called shin splints is inflammation of soft tissues that connect to the tibia (shin) from too much pounding/impact or improper technique with impact (running and landing). A stress fracture is an injury inside the bone rather than only at its “skin” (periosteum). Stress fractures can be caused from similar things as MTSS.

Risks for both: MTSS and Stress Fractures
While there are many differences between MTSS and stress fractures, there are also some common causes. Let's take a look at risks for developing both conditions.1. Running surface
Softer is better, if a runner on a track – don’t run only clockwise, some days run counter clock wise. Change “Good” running shoes every 400 miles or every 6 months - whichever occurs first. If you are a gymnast: use tumble track when possible, use shoes during warm up and conditioning, watch your numbers on Vault and Floor
2. Landings
When running, run heel to toe rather than flat footed. If you can hear a “stomp”, this could be a risk.
Dismounts: Land “softly” with knees bent and ankles helping to absorb impact rather than only feet. Avoid “short landings” and “crunching” which can add stress to shins.
3. Overuse
Watch numbers. When a runner is experiencing pain, they should consider decreasing mileage. For a gymnast, this would translate into reducing repetitions and hard landings - especially on tumbling passes and vaults.
4. Kinetic chain
Are your hips, knees, and ankle/feet incorrectly positioned when running causing added stress to the shins? A Physical Therapist can help with a running analysis. (Learn how to choose a physical therapist for your athlete here.)
5. Flexibility
Hamstring, quadriceps, Achilles and calf muscles that are tight can result in unwanted stress to the shin.
6. Diet/Hormones
Protein intake and enough calories: a young athlete needs more calories (than a non athlete) for their sport, as well as normal development at their age - to have the ability to increase strength (muscle) and help heal injuries.
Estrogen levels in women and testosterone levels in men are “bone strengtheners”. In females, a problem with menstrual cycles can increase risk for stress fractures
How Do I Know If I Have Shin Splints (MTSS)?
Medial Tibial Stress Syndrome (MTSS) once called shin splints is inflammation of soft tissues that connect to the tibia (shin) from too much pounding/impact or improper technique with impact (running and landing).
-
Pain is typically a “strip” of pain down the length of the medial (inside) shin bone.
-
OPTIONAL testing : Xray will be normal, MRI often will show inflammation of the connective tissue to the shin and at the “skin of the bone” (the periosteum)- but no inflammation (or edema) inside the tibia (the shin bone).
-
Treatment is stretching, good running technique, decrease frequency of pounding/impact, ice, good shoe wear, and cautious use of NSAIDS (like Aleve). PT for a running analysis and kinetic chain analysis should be considered to decrease recurrences.
-
Some athletes benefit from taping the shins, topical compounding cream, deep tissue massage, cold laser- but what might work for one athlete may not seem to help another with the same diagnosis.
-
It is ok to modify activity (decrease amount) and continue if skills are safe (not limping) and the pain is decreasing with treatment.
How Do I Know If I Have a Stress Fracture In My Tibia?
A stress fracture is an injury inside the bone rather than only at its “skin” (periosteum). Stress fractures can be caused from similar things as MTSS.
- Pain is more likely to be in a point tender area of the medial (inside) tibia (shin) rather than a strip of pain. While MTSS often improves a bit once “warmed up”, stress fractures tend to worsen through a practice. Pain when “not doing anything” is also a possibility with a stress fracture (and not usually with MTSS (shin splints))
- REQUIRED testing: Xray is the first test (and sometimes shows thickening at the bone suggesting the bone is trying to heal) but if xray is normal MRI can still pick up a developing / small / or not seen on xray stress fracture – inside the shin bone (tibia). If the xray shows the problem MRI is not usually needed. If the xray does not reveal the problem- at least consider MRI as it is more sensitive than xray.
- Treatment is NO IMPACT (usually a boot and sometimes crutches too) for 6 weeks usually.
- Physical therapy after the rest period to help decrease recurrence by evaluating the running / landing / impact of the athlete and ensure there isn’t anything in the technique that is a risk.
- It is NOT OK to continue impact/pounding (on the injured side) with a diagnosis of a stress fracture. Consider swimming, upper body only conditioning, or “anti gravity treadmill” during treatment time.
- Rarely, if rest and booting alone doesn’t work, crutches, EXOGEN bone stimulator, medication, diet alterations, and as a last resort - surgery is considered.
- If an athlete has had more than one stress fracture in their life- then a special work up is considered to see if they are at risk for having “weaker bones” than other athletes their age doing the same skills. Problems may include anemia, thyroid disorders, vitamin D deficiency, hormone abnormalities, a metabolic bone disorder, etc. Blood tests and a DEXA bone density are often considered in this work up.
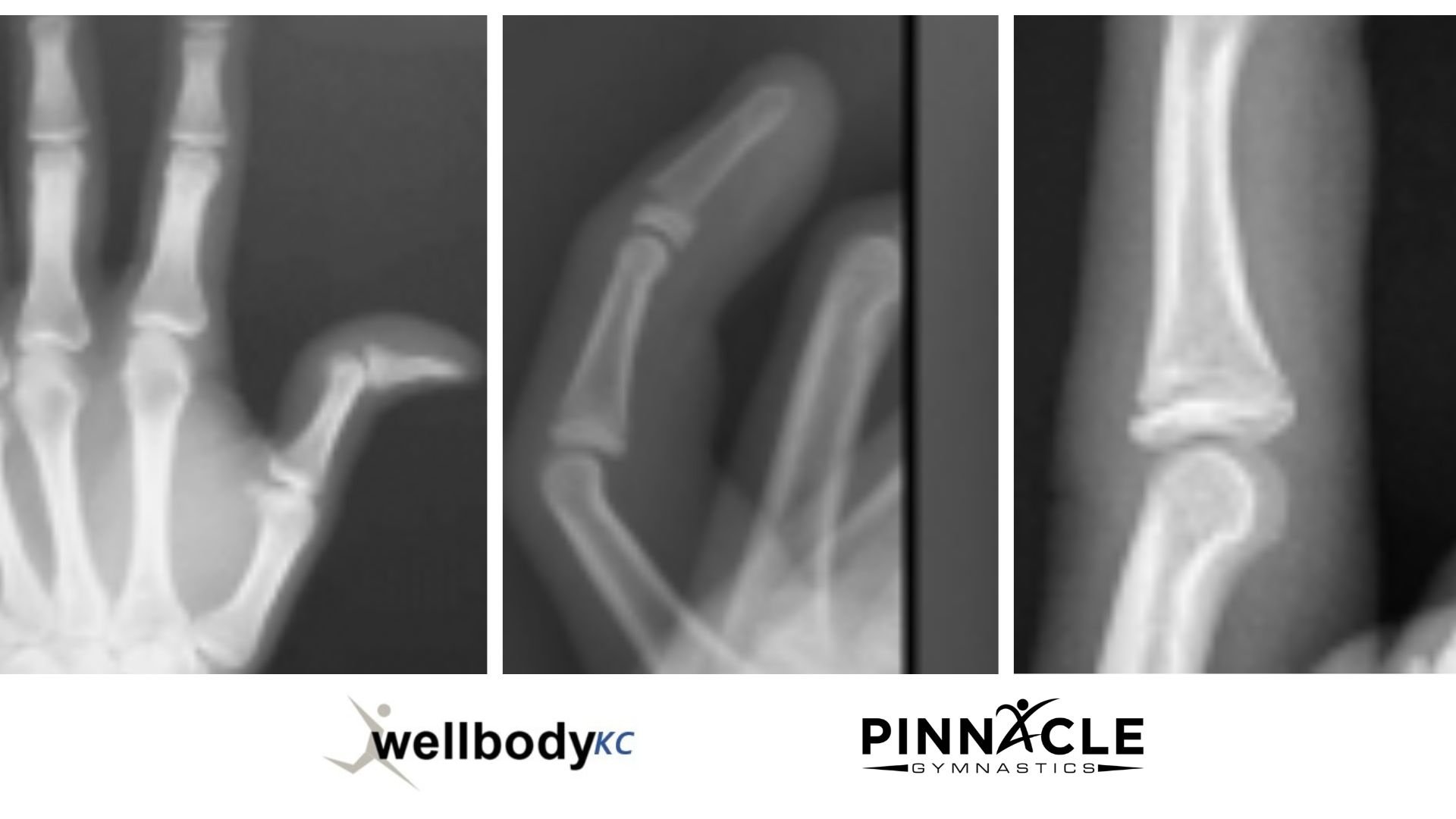
The Radiology of Shin Splints vs. Tibia Stress Fracture
A doctor is the best person to determine if the injury is a stress fracture or MTSS. Upon seeing the doctor, a physical exam will be necessary to determine if radiology imaging is required to diagnose.
1. Work Up
A sports doctor will evaluate your levels and placement of pain to determine the best way to progress back to full impact. If the physical exam leads the doctor to suspect a stress fracture, he will order imaging to confirm the diagnosis.
2. Radiology
MTSS and tibia stress fractures can be seen through both x-ray and MRI. Always consider using a sports doctor familiar with the athlete's sport, level, and age group when diagnosing any sports related injury or condition. If the imaging supports a stress fracture, the athlete will be removed from impact until the injury can heal. Once healed, the athlete will need to participate in physical therapy in order to return safely to sport and full strength.
View an example of Radiologic Abnormalities for MTSS and Stress Fractures of Tibia here.
Board Certified Pediatrician with an interest in Sports Medicine
Concussion Management Team
Team Medicine